The COVID-19 pandemic has sharply focussed interest on the role of nutrition in immune health and has sparked a plethora of media stories suggesting that certain foods and supplements are capable of ‘boosting’ the immune system, with sales of vitamin and mineral supplements rising sharply.
But even before COVID-19, there has long been an association between food and immunity – when people want to stave off or fight common illnesses such as colds and flu they may turn to particular foods like chicken soup, honey and garlic or rush to take vitamin C and zinc supplements to improve immunity. But can these really ‘boost’ our immune system?
Contributed by Helena Gibson-Moore, Nutrition Scientist and Ayela Spiro, Nutrition Science Manager
Be careful of myths and false promises!
Despite popular media suggesting that certain food components and supplements can ‘boost’ the immune system, we need to acknowledge that our immune function is influenced by many factors, not just diet, and not by any one specific food or nutrient alone – a healthy lifestyle including enough sleep and physical activity and low stress levels are all important to support immunity. But adequate energy and a range of nutrients are needed to help support normal immune function
How do nutrients play a part?
The role of nutrients in immunity is a fascinating one. Our immune system is complex and involves an intricate network of specialised cells and communicating molecules that work together to defend the body against attacks from pathogens like harmful bacteria, viruses, and parasites. Our innate and adaptive immune systems work together; the innate immune system provides fast and non-specific immune responses, mediated by cells such as monocytes whilst the adaptive system provides a highly specific response mediated by T and B cells. In addition, a complement system ( a complex series of blood proteins that act in a cascade to “complement” the role of immune cells drive inflammation and destroy pathogen cells.
Adequate appropriate nutrition is required for all cells to function normally, and this includes the cells in the immune system, but an activated immune response further increases the demand for energy and many nutrients. Both macro and micronutrients and dietary components have very specific roles in the development and maintenance of an effective immune system throughout the life course. For example, amino acids, the building blocks of proteins, are required in the synthesis of chemicals involved in the immune response and omega-3 fatty acids may influence inflammation and immune function through a variety of mechanisms. An array of micronutrients (e.g. vitamins A, D, C, E, B6, B12 and folate and the minerals zinc, iron, copper and selenium) are needed for innate and cell mediated immunity, and for protection against oxidative and inflammatory stress – see Table 1 for examples of foods that provide these nutrients. We also know that dietary factors like fibre affects our gut microbiota which has a role in immune regulation. The wide range of nutrients that play a role in immunity demonstrates the importance of a balanced and varied diet for maintaining a healthy immune system.
Table 1: Nutrients that help support the normal function of the immune system and some of their food sources
| Vitamin A | Vitamin B6 | Vitamin B12 | Vitamin C | Vitamin D |
|---|---|---|---|---|
|
Liver, eggs and cheese [sources of retinol ("pre-formed" vitamin A)]. Dark green leafy vegetables and orange-coloured fruits and vegetables [e.g. carrots, sweet potato, butternut squash, cantaloupe melon, and spinach as carotenoids (converted to vitamin A by the body)] |
Poultry, some fish, fortified breakfast cereals, egg yolk, soya beans, and some fruit and vegetables, such as banana, avocado, and green pepper. | Red meat, fish, shellfish, milk, cheese, eggs, yeast extract, fortified dairy alternatives and fortified breakfast cereals. | Citrus fruits, blackcurrants, strawberries, papaya, kiwi, green vegetables, e.g. broccoli, peppers and tomatoes. | Oily fish (e.g. salmon, mackerel), eggs, some fortified breakfast cereals, fortified spreads and some fortified dairy products and alternatives. |
| Copper | Folate | Iron | Selenium | Zinc |
|---|---|---|---|---|
| Brown and wholemeal bread, wheat-based breakfast cereals, quinoa, shellfish, pulses, avocado, dried fruit, nuts and seeds. | Green vegetables (e.g. cabbage), pulses, oranges, berries, nuts, some cheeses, brown and wholemeal bread, and fortified breakfast cereals. | Offal, red meat, some pulses (e.g. lentils, haricot beans), nuts, some sea food (canned sardines, cockles, mussels), quinoa, brown and wholemeal bread and some dried fruit (e.g. raisins, semi-dried apricots). | Nuts and seeds (for example Brazil nuts, cashews and sunflower seeds), eggs, offal, poultry, fish and shellfish. | Meat, pultry, cheese, some shellfish, nuts and seeds (e.g. pumpkin seeds, pine nuts), wholegrain and seeded breads. |
*The evidence on these nutrients and their association with the immune system has been reviewed by the European Food Standards Authority (EFSA) and the following authorised health claim relates to each of them: ‘contributes to the normal function of the immune system’.
Source: Authorised health claims: Great Britain NHC register, EU Register of Health Claims
Micronutrient deficiency and immunity
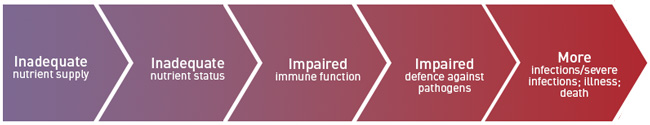
The dangerous impact of micronutrient deficiencies on the immune system can be seen from their severe health consequences in developing countries – for example zinc deficiency increases susceptibility to infections such as diarrhoea, pneumonia and malaria, vitamin A deficiency increases the risk of disease and death from infections (diarrhoea, measles) and iron deficiency anaemia increases the risk of bacterial infection during childbirth (see the diagram below which illustrates how inadequate nutrition cascades to adverse effects on immunity).
It’s important to note that whilst deficiency is associated with adverse outcomes, the opposite assumption that more must equal better, does not follow and high dose supplementation of certain micronutrients can also have adverse implications on health.
Spotlight on vitamin D
The discovery of vitamin D receptors and vitamin D metabolic enzymes in immune cells has provided much interest in the role of this vitamin in immunity. During the COVID-19 pandemic this has increased, particularly in light of a suggested link between vitamin D and risk of acute respiratory tract infections (ARTI). However, evidence on vitamin D and ARTI risk does not necessarily extrapolate to COVID-19, the infectious disease caused by severe acute respiratory syndrome coronavirus 2 virus (SARS-CoV-2). Indeed, the National Institute for Health and Care Excellence (NICE), the organisation that provides national guidance to improve health and social care in the UK, in its Rapid guideline on COVID-19 vitamin D recognised that, as yet, there is no robust evidence to recommend vitamin D supplementation solely to prevent or treat COVID 19. The current UK recommendation to take a 10 micrograms vitamin D supplement in the autumn/winter months is based on evidence of its importance in protecting musculoskeletal health.
The gut microbiome and immunity
The gut microbiome is associated with a role in the immune system and is suggested to enhance immunity both locally in the gut and more systemically in the body, although this remains poorly understood. Our gut microbiome is influenced by factors such as age, disease status and antibiotic use but also by our dietary intake. This has prompted interest in whether probiotics could be used to influence immunity, although considerable inconsistency between studies including strain specific differences or doses and individual variability make it difficult to make any conclusive recommendations in terms of pre/probiotics. A good way to promote a healthy gut microbiome is to include a wide variety of high-fibre plant-based foods like fruit and vegetables, wholegrains, nuts, seeds, beans, peas and lentils.
The Overall Message
No one food or supplement, or specific diet can support the immune system alone. However, eating a healthy diet that contains plenty of wholegrains, fruit and vegetables (as well as taking vitamin D supplements as per health expert advice), managing stress, being physically active and getting enough sleep will help the immune system to work properly. Being underweight or overweight can also contribute to a weakened immune system. When looking for information on diet and health it is important to seek evidence-based advice from authoritative sources. And making sure that we have all the nutrients the body needs is important not only for supporting our immunity in respect of COVID-19 but for other aspects of health too.
More information about the British Nutrition Foundation, and about nutrition and health can be found on the Foundation’s website www.nutrition.org.uk
References
- Calder PC. Nutrition, immunity and COVID-19. BMJ Nutrition, Prevention & Health 2020
- Lockyer S. Effects of diets, foods and nutrients on immunity: Implications for COVID‐19? Nutrition Bulletin 2020;45(4):456-473
- NICE. COVID-19 rapid guideline: vitamin D (NG187) https://www.nice.org.uk/guidance/ng187
- Scientific Advisory Committee on Nutrition (2015) Carbohydrates and Health. https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/445503/SACN_Carbohydrates_and_Health.pdf
- Childs CE, Calder PC, Miles EA. Diet and immune function. Nutrients 2019;11:1933.
- Hill C, Guarner F, Reid G et al. Expert consensus document: The International Scientific Association for Probiotics and Prebiotics consensus statement on the scope and appropriate use of the term probiotic. Nature Reviews Gastroenterology and Hepatology 2014;11:506
- NHS. Probiotics https://www.nhs.uk/conditions/probiotics/
- Collinson S, Deans A, Padua-Zamora A et al. Probiotics for treating acute infectious diarrhoea. Cochrane Database of Systematic Reviews 2020;12:CD003048
- Padhani ZA, Moazzam Z, Ashraf A et al. Vitamin C supplementation for prevention and treatment of pneumonia. Cochrane Database of Systematic Reviews 2020;4:CD013134
- Hemila H, Chalker E. Vitamin C for preventing and treating the common cold. Cochrane Database of Systematic Reviews 2013:CD000980.
- Lassi ZS, Moin A, Bhutta ZA. Zinc supplementation for the prevention of pneumonia in children aged 2 months to 59 months. Cochrane Database of Systematic Reviews 2016;12:CD005978
- Wang L, Song Y. Efficacy of zinc given as an adjunct to the treatment of severe pneumonia: a meta-analysis of randomized, double-blind and placebo-controlled trials. Clinical Respiratory Journal 2018;12:857–64
- Joachimiak MP. Zinc against COVID-19? Symptom surveillance and deficiency risk groups. PLOS Neglected Tropical Diseases 2021;15(1):e0008895
- NIH (National Institutes of Health) Coronavirus Disease (COVID-19) Treatment Guidelines. Zinc supplementation and COVID-19 https://www.covid19treatmentguidelines.nih.gov/adjunctive-therapy/zinc/
- NIH (National Institutes of Health) Coronavirus Disease (COVID-19) Treatment Guidelines. Vitamin C https://www.covid19treatmentguidelines.nih.gov/adjunctive-therapy/vitamin-c/
- Sattar N, McInnes IB, McMurray JJ. Obesity a risk factor for severe COVID-19 infection: multiple potential mechanisms. Circulation 2020;142:4-6
- Dicker D, Bettini S, Farpour-Lambert N et al. Obesity and COVID-19: The Two Sides of the Coin. Obesity Facts 2020;13(4):430-438
- Robinson E, Gillespie S, Jones A. Weight-related lifestyle behaviours and the COVID-19 crisis: An online survey study of UK adults during social lockdown. Obesity Science & Practice 2020;6(6):735-740

Nutrition plays a key role in consumers’ lives
We address the health and nutritional needs of your consumers using our science-based innovative ingredient solutions. Discover how in our Nutrition Centre...